Information for Patients
Understanding there are fertility preservation options available and seeing a reproductive specialist in a timely manner can improve your emotional outlook and future quality of life.
Introduction
Many women who have been diagnosed with cancer think preserving their fertility is important and want information about their options. However,
- You may not feel comfortable bringing up fertility issues.
- You may not be aware of your options for preserving fertility.
- You may be focused on your cancer diagnosis and unable to think about fertility or the possibility of having a future family.
You may later regret not considering fertility issues prior to starting cancer treatment.
Even women with a poor prognosis may want to consider fertility preservation.
Ask Your Doctor
These key points can help start the conversation:
- How will my cancer and cancer treatment affect my fertility?
- Based on my treatment plan, what is my risk of infertility [high, moderate, low]?
- What are my options for fertility preservation before I begin cancer treatment (see table below)?
- Can you refer me to a fertility preservation specialist to discuss my options further?
The American Society of Clinical Oncology and American Society for Reproductive Medicine recommend, when possible, at-risk patients should see a fertility preservation specialist prior to starting cancer treatment.
The following table gives a brief description of options available to women who wish to preserve their fertility. Discuss available options with your doctor.
Several resources are listed below and can help you locate a fertility preservation specialist.
Remember there are other ways to build a family after cancer if you are unable to preserve your fertility now. Talking with a specialist can help you explore other options that might be right for you.
Fertility Preservation - Where Does It Fit?
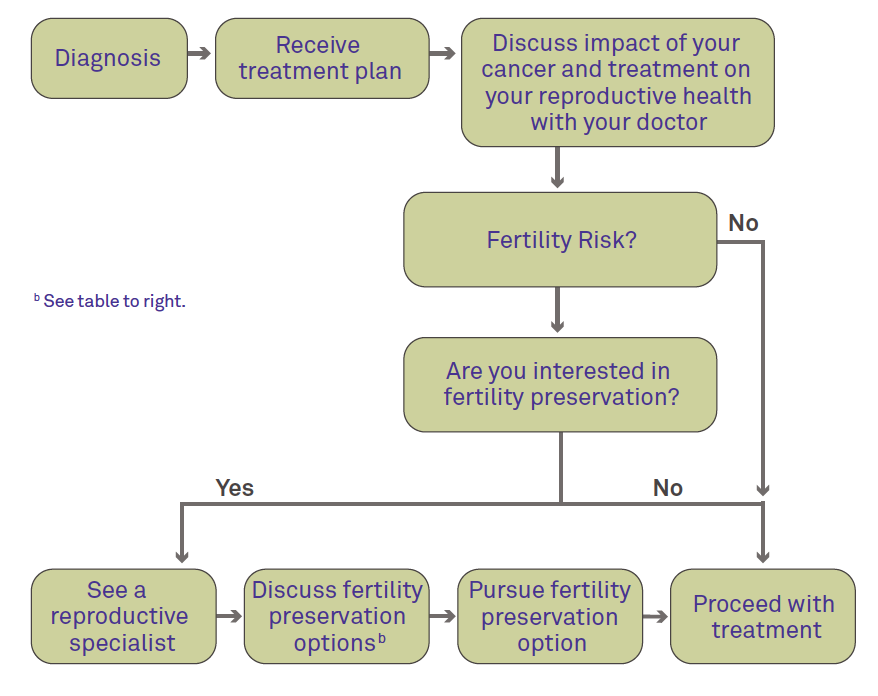
Options for Fertility Preservation
| Option | Definition | Timing | Time Requirement | Other Considerations |
|---|---|---|---|---|
|
Embryo Banking
|
Ovarian stimulation; Harvesting eggs, IVF and freezing of embryos | Before or after treamtment | 10-15 days outpatient surgical procedure | Need partner or sperm donor |
| Egg Banking | Ovarian stimulation; Harvesting and freezing of unfertilized eggs | Before or after treamtment | 10-15 days outpatient surgical procedure | |
| Ovarian Tissue Banking (Experimental) | Surgical removal of ovarian tissue and processing of tissue for freezing | Before or after treamtment | Outpatient surgical procedure | Autotransplantation of tissue has produced live births; studies ongoing for IVFM |
| Radiation Shielding | Use of shielding to reduce scatter radiation to the ovaries | During treatment | In conjunction with radiation treatments | Does not protect against effects of chemotherapy |
| Ovarian Transposition | Surgical reposition of ovaries out of radiation field | Before treatment | Outpatient procedure | |
| Radical Trachelectomy | Surgical removal of the cervix with preservation of the uterus | Before treatment | Inpatient surgical procedure | Limited to early stage cervical cancer |
| Ovarian Suppression (Experimental) | GnRH analogs used to suppress ovaries | During treatment | In conjunction with chemotherapy | Data are mixed on the effectiveness of this option. |
Resources
For more information about infertility risk and fertility preservation options for men diagnosed with cancer:
- Visit SaveMyFertility.org
- Call the FERTLINE: 866-708-FERT (3378)
- Visit the Oncofertility Consortium® Web site
- Use the online Clinic/Center Finder to find the fertility preservation center closest to you.
- Visit the Patient Navigator Website
References
- The Ethics Committee of the American Society for Reproductive Medicine. Fertility preservation and reproduction in patients facing gonadotoxic therapies: a committee opinion. Fertil Steril. 2013; 100:1224-31.
- De Vos M, Smitz J, Woodruff TK. Fertility preservation in women with cancer. Lancet. 2014;384:1302-10.
- Jeruss JS, Woodruff TK. Preservation of fertility in patients with cancer. N Engl J Med. 2009;360:902-911.
- Loren AW, et al. Fertility preservation for patients with cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol. 2013; 31: 2500-10.
- Meirow D, Biederman H, Anderson RA, Wallace WH. Toxicity of chemotherapy and radiation on female reproduction. Clin Obstet Gynecol. 2010;53:727-739.
- JM Letourneau, EE Ebbel, PP Katz, et al. Pretreatment fertility counseling and fertility preservation improve quality of life in reproductive age women with cancer. Cancer. 2012; 118:1710–1717.
- Levine JM, Kelvin JF, Quinn GP, Gracia CR. Infertility in reproductive-age female cancer survivors. Cancer. 2015;121(10):1532-9.
- Tschudin S, Bitzer J. Psychological aspects of fertility preservation in men and women affected by cancer and other life-threatening diseases. Hum Reprod Update. 2009;15:587-597.
- Woodruff TK. The Oncofertility Consortium—addressing fertility in young people with cancer. Nat Rev Clin Oncol. 2010;7:466-475.

