Information for Providers
Many men who have been diagnosed with cancer think preserving their fertility is important and want information about their options.
Introduction
Understanding that there are fertility preservation options available and referring at-risk patients in a timely manner to reproductive specialists can improve patients’ emotional outlook and future quality of life. However,
- Patients may not feel comfortable bringing up fertility issues.
- Patients may not be aware of their options for preserving fertility.
- Patients may be focused on their cancer diagnosis and unable to think about fertility or the possibility of having a future family.
- Even men with a poor prognosis may want to consider fertility preservation.
- Men may later regret not considering fertility issues prior to starting cancer treatment.
Fertility Preservation - Where Does It Fit?
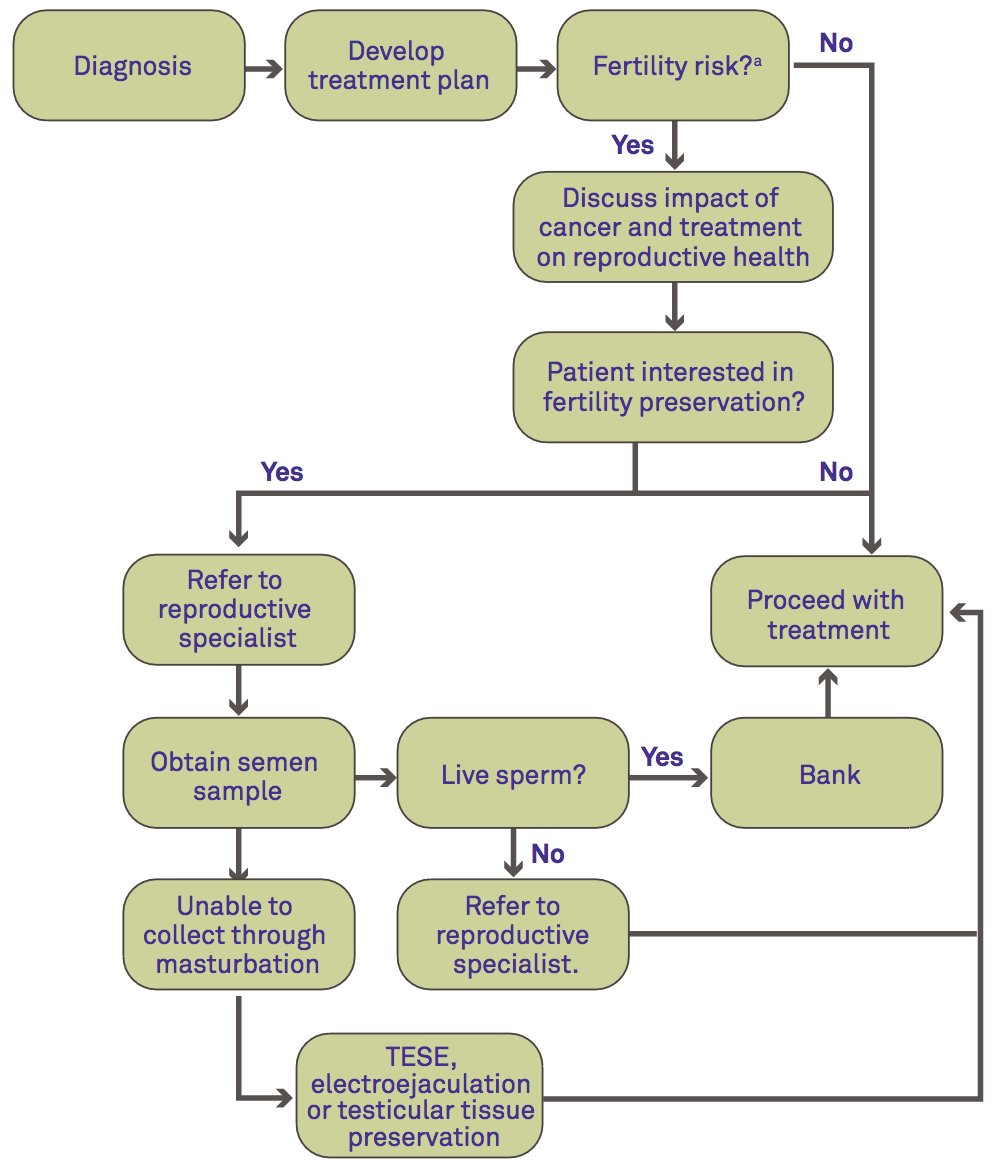
Figure adapted from Brannigan RE. Cancer Treat Res. 2007;138:28-49.
a) See table below
b) See figure below
Starting the Conversation
Discussing fertility preservation is important. These key points can help start the conversation:
- Cancer and cancer treatment may affect your fertility.
- Based on your treatment plan, your risk of infertility is [high, moderate, low] (see table on reverse).
- Although it may not be on your mind now, it is important to discuss fertility before you begin treatment. You may have options for fertility preservation before you begin cancer treatment (see figure to right).
- I can refer you to a fertility preservation specialist if you would like to discuss your options further.
- Remember there are other ways to build a family after cancer if we are unable to preserve your fertility now. Talking with a specialist can help you explore other options that might be right for you.
Options for Fertility Preservation
- The American Society of Clinical Oncology and the American Society for Reproductive Medicine recommend, when possible, at-risk patients be referred to a fertility preservation specialist prior to starting cancer treatment.
- There are standard options for men diagnosed with cancer who wish to preserve their fertility. These options are illustrated in the figure below.

Figure adapted from Brannigan RE. Cancer Treat Res. 2007;138:28-49.
Cancer Therapy and the Risk of Infertility
Individual chemotherapeutic agents and multi-agent regimens are associated with varying degrees of infertility risk.
While this table provides general guidelines, each patient is different and treatment may impair their fertility differently.
| High Risk |
|
|---|---|
| Intermediate Risk |
|
| Low Risk |
|
| Very Low / No Risk |
|
| Unknown Risk |
|
Table adapted from LIVESTRONG; and Brannigan RE. Cancer Treat Res. 2007;138:28-49.
MOPP=mechlorethamine/oncovin (vincristine)/procarbazine/prednisone • MVPP=mechlorethamine/vinblastine/procarbazine/prednisolone • COPP=cyclophosphamide/oncovin/procarbazine/prednisone • ChlVPP=chlorambucil/vinblastine/procarbazine/prednisolone • EVA=etoposide/vinblastine/adriamycin (doxorubicin) • ABVD=adriamycin/bleomycin/vinblastine/dacarbazine • BEP= bleomycin/etoposide/cisplatin • OEPA=oncovin/etoposide/prednisone/adriamycin (doxorubicin) • NOVP=novantrone (mitoxantrone)/oncovin/vinblastine/prednisone • CHOP=cyclophosphamide/hydroxydaunomycin/oncovin/prednisone • COP=cyclophosphamide/oncovin/prednisone
Resources
For more information about infertility risk, fertility preservation options for women diagnosed with cancer, and how to locate and refer your patients to a fertility preservation specialist:
- Visit SaveMyFertility.org
- Call the FERTLINE: 866-708-FERT (3378)
- Visit the Oncofertility Consortium® Web site
- Use the online Clinic/Center Finder to find the fertility preservation center closest to you.
References
- Brannigan RE. Fertility preservation in adult male cancer patients. Cancer Treat Res. 2007;138:28-49.
- Brannigan RE. Risk of infertility in male survivors of childhood cancer. Lancet Oncol. 2014; 15(11): 1181-2.
- Osterberg EC, Ramasamy R, Masson P, Brannigan RE. Current practices in fertility preservation in male cancer patients. Urol Ann. 2014; 6(1): 13-17.
- The Ethics Committee of the American Society for Reproductive Medicine. Fertility preservation and reproduction in patients facing gonadotoxic therapies: a committee opinion. Fertil Steril. 2013; 100:1224-31.
- Jeruss JS, Woodruff TK. Preservation of fertility in patients with cancer. N Engl J Med. 2009;360:902-911.
- Loren AW, et al. Fertility preservation for patients with cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol. 2013; 31: 2500-10.
- Tschudin S, Bitzer J. Psychological aspects of fertility preservation in men and women affected by cancer and other life-threatening diseases. Hum Reprod Update. 2009;15:587- 597.

