Information for Patients
Many adult survivors of childhood cancer feel fertility preservation and the ability to have a future family are important.
Understanding there may be fertility preservation options available and having your child see a reproductive specialist in a timely manner can improve their future quality of life.
Introduction
You may not be aware there are options for preserving fertility in your child diagnosed with cancer.
- You may be focused on cancer treatment and your child’s immediate health.
- You may feel uncomfortable discussing issues of reproduction with your child.
Ask Your Doctor
Discussing fertility preservation is important. These key points can help start the conversation:
- Cancer and cancer treatment may affect my child’s fertility.
- Will my child’s cancer or cancer treatment affect his/her fertility?
- What are the options to try to preserve my child’s fertility before he/she begins cancer treatment (see figure below).
- Can you refer us to a fertility preservation specialist to discuss my child’s options further?
Fertility Preservation - Where Does It Fit?
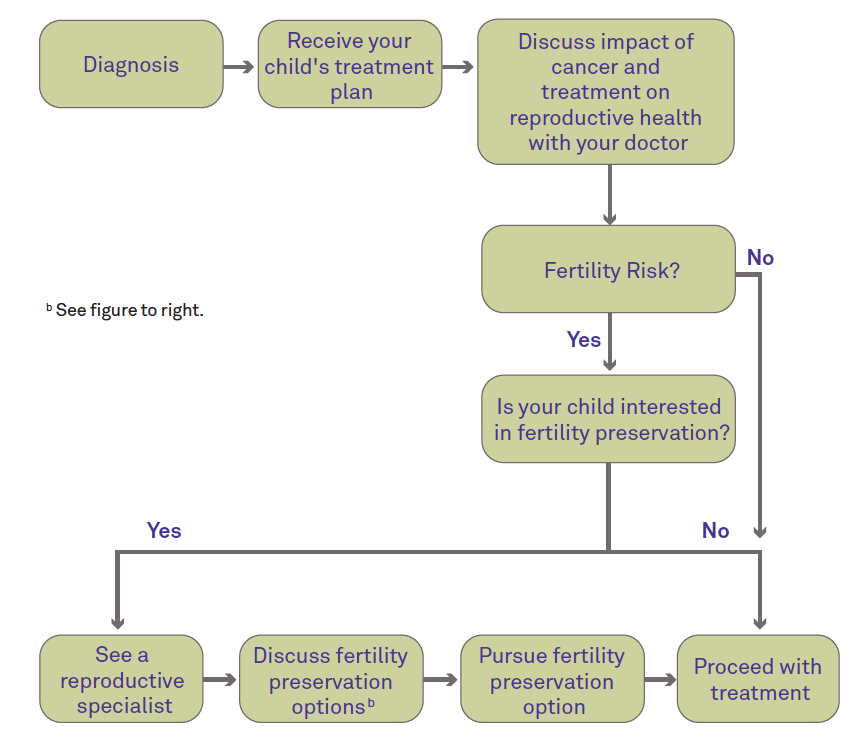
Options for Fertility Preservation
- The following diagram gives a brief description of fertility preservation options available to children diagnosed with cancer before and after treatment.
- There are several resources listed on the reverse that can help you locate a fertility preservation specialist to discuss your child’s options.
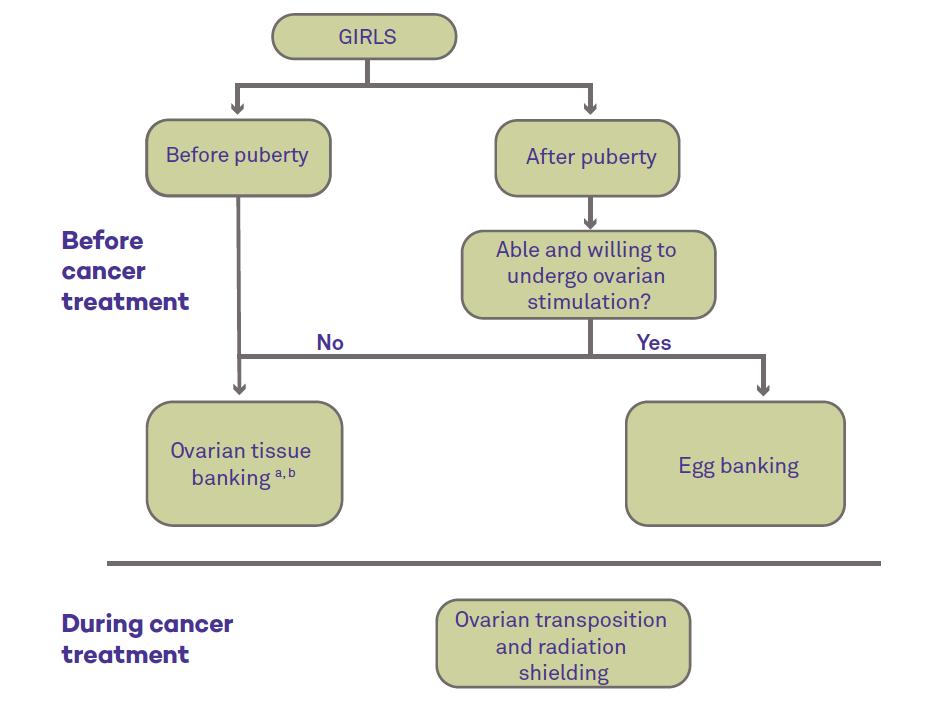
a Not an option if there is a high risk of ovarian metastases. Discuss with your doctor.
b Experimental—only performed as part of a clinical study approved by an IRB.
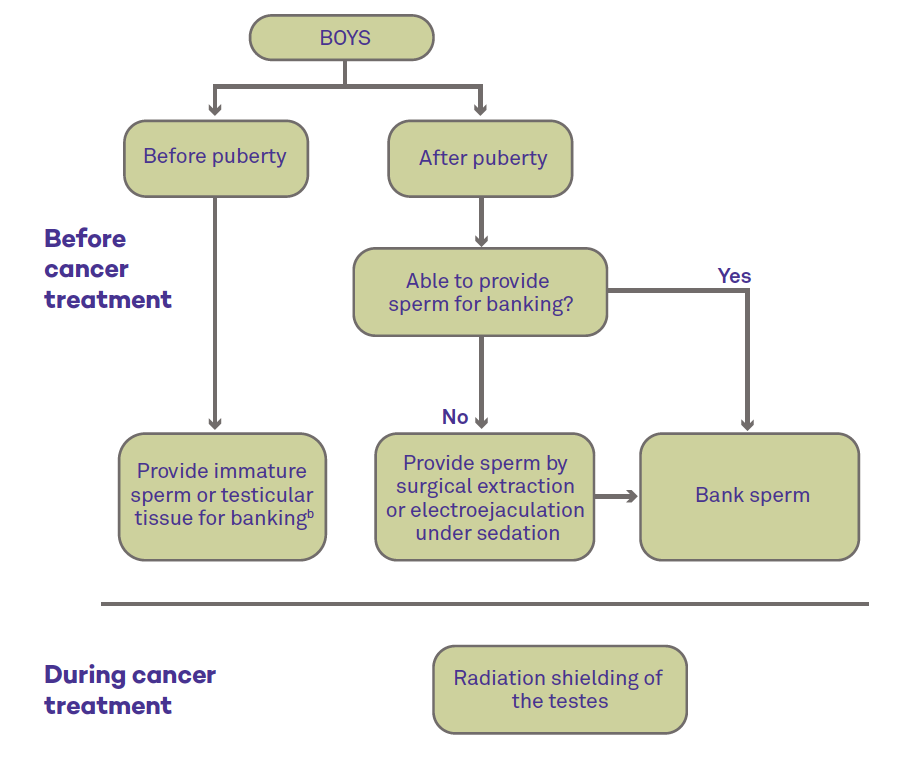
Resources
For more information about infertility risk and fertility preservation options for children diagnosed with cancer:
- Visit SaveMyFertility.org
- Call the FERTLINE: 866-708-FERT (3378)
- Visit the Oncofertility Consortium Web site
- Use the online Clinic/Center Finder to find the fertility preservation center closest to you
- Visit the Pediatric Oncofertility Research Foundation
- Visit the Patient Navigator Website
References
- The Ethics Committee of the American Society for Reproductive Medicine. Fertility preservation and reproduction in patients facing gonadotoxic therapies: a committee opinion. Fertil Steril. 2013; 100:1224-31.
- Chow EJ, et al. Pregnancy after chemotherapy in male and female survivors of childhood cancer treated between 1970 and 1999: a report from the Childhood Cancer Survivor Study cohort. Lancet Oncol. 2016;17(5):567-76.
- Ginsberg JP. New advances in fertility preservation for pediatric cancer patients. Curr Opin Pediatr. 2010;23:9-13.
- Long CJ, Ginsberg JP, Kolon TF. Fertility Preservation in Children and Adolescents With Cancer. Urology. 2016;91:190-6.
- Loren AW, et al. Fertility preservation for patients with cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol. 2013; 31: 2500-10.
- Nieman CL, et al. Fertility preservation and adolescent cancer patients: lessons from adult survivors of childhood cancer and their parents. Cancer Treat Res. 2007;138:201-217.
- Redig AJ, Brannigan R, Stryker SJ, et al. Incorporating fertility preservation into the care of young oncology patients. Cancer. 2010;117:4-10.

